In developing countries, home-based HIV testing and counseling (HBHTC) is an emerging approach for addressing confidentiality issues. 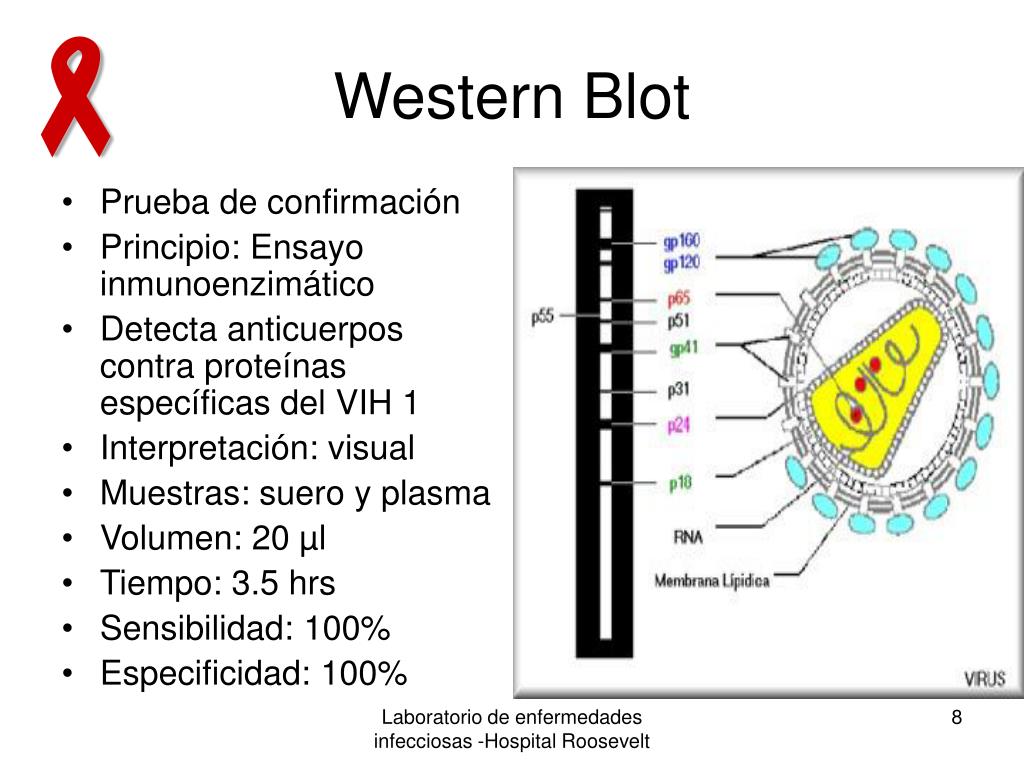
This allows for monitoring of infected individuals easily, compared to anonymous testing that has a number attached to the positive test results. More state funded testing sites are now using confidential forms of testing. Some legal jurisdictions permit such disclosure, while others do not. Conducted with the informed consent of the person being tested.Ĭonsiderable controversy exists over the ethical obligations of health care providers to inform the sexual partners of individuals infected with HIV that they are at risk of contracting the virus.Accompanied by counseling (for those who test positive).According to these principles, the conduct of HIV testing of individuals must be The UNAIDS/WHO policy statement on HIV Testing states that conditions under which people undergo HIV testing must be anchored in a human rights approach that pays due respect to ethical principles. The combination of these two methods is highly accurate Human rights If antibodies are detected by an initial test based on the ELISA method, then a second test using the western blot procedure determines the size of the antigens in the test kit binding to the antibodies. In the United States, this is achieved using an algorithm combining two tests for HIV antibodies. Tests used for the diagnosis of HIV infection in a particular person require a high degree of both sensitivity and specificity. As of 2001, the risk of transfusion-acquired HIV in the US was approximately one in 2.5 million for each transfusion. These diagnostic tests are combined with careful donor selection. In the US, the Food and Drug Administration requires that all donated blood be screened for several infectious diseases, including HIV-1 and HIV-2, using a combination of antibody testing ( EIA) and more expeditious nucleic acid testing (NAT). The World Health Organization estimated that, as of 2000, inadequate blood screening had resulted in 1 million new HIV infections worldwide. A combination of antibody, antigen and nucleic acid tests are used by blood banks in Western countries. Tests selected to screen donor blood and tissue must provide a high degree of confidence that HIV will be detected if present (that is, a high sensitivity is required). Principles Screening donor blood and cellular products Most false negative results are due to the window period. Autoimmune diseases, such as systemic lupus erythematosus, have also rarely caused false positive results. Nonspecific reactions, hypergammaglobulinemia, or the presence of antibodies directed to other infectious agents that may be antigenically similar to HIV can produce false positive results. False negative: The test incorrectly indicates that HIV is absent in an infected person. 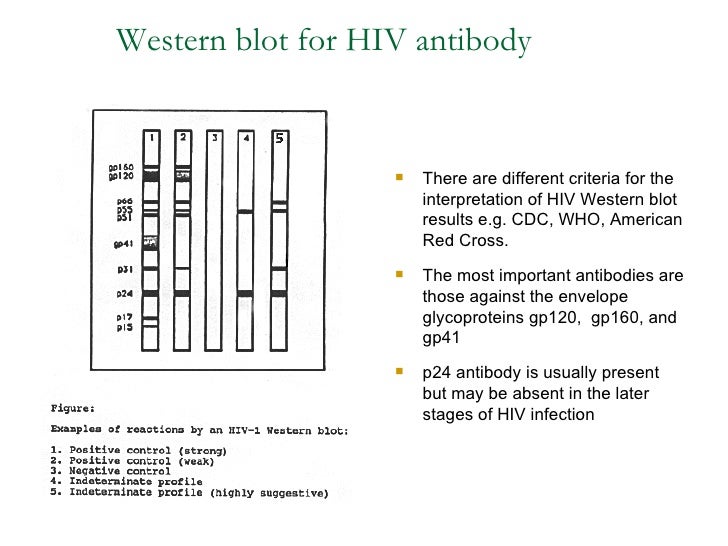
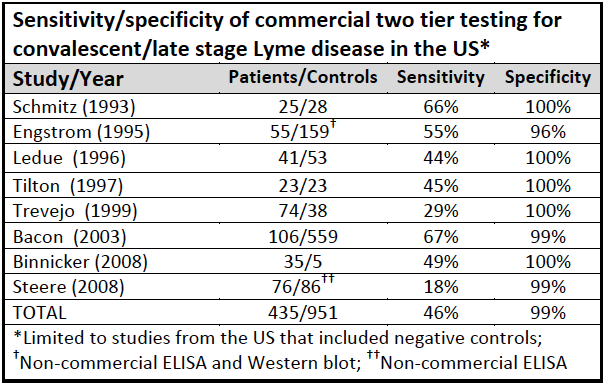
False positive: The test incorrectly indicates that HIV is present in a non-infected person.Specificity: The percentage of the results that will be negative when HIV is not present.Īll diagnostic tests have limitations, and sometimes their use may produce erroneous or questionable results.Sensitivity: The percentage of the results that will be positive when HIV is present.Performance of medical tests is often described in terms of: Antigen testing cuts the window period to approximately 16 days and nucleic acid testing (NAT) further reduces this period to 12 days. The average window period with HIV-1 antibody tests is 25 days for subtype B. The window period is the time from infection until a test can detect any change. Main article: AIDS-defining clinical condition 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
